- Or what happened when my friend broke her wrist near Mt Feathertop
- Doing (and re-doing) remote area first aid courses helps you:
- Here’s the process that we went through to get her to medical help.
- What did we consider in making a plan?
- In Margot's own words...
- What’s the difference between a standard Senior First Aid course and one that is specific for Wilderness or Remote Area First Aid?
- What's in my first aid kit?
- Buy an emergency communications device
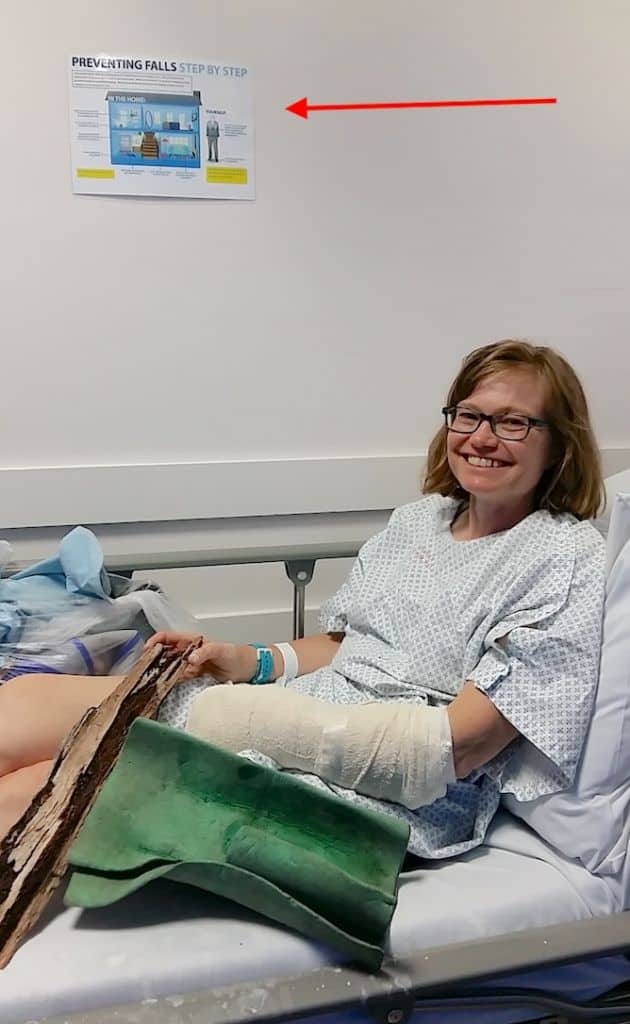
Or what happened when my friend broke her wrist near Mt Feathertop

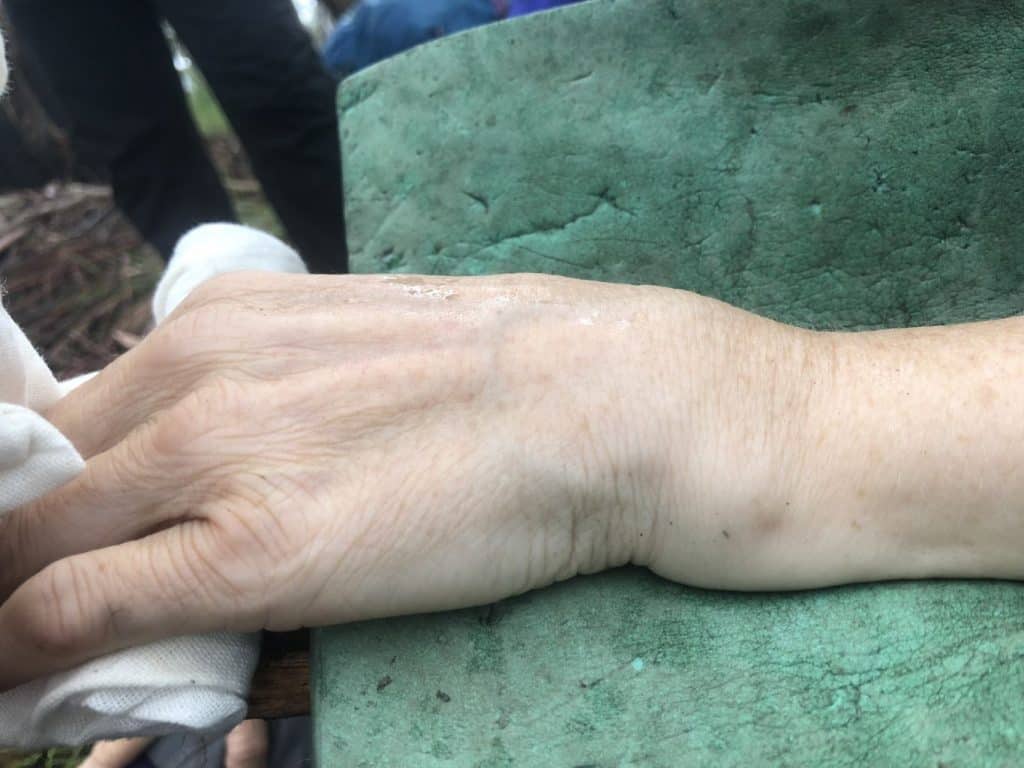
* Warning: Cringe-worthy photos of broken bones below – don’t scroll if squeamish!
Slip, drop, SNAP! That’s how our fourth day in the stunning Victorian High Country changed its course from one of a simple final descent to the trailhead, to something quite other.
After hearing one of my fellow walkers call my name, I looked up to see only Margot’s backpack lying on the ground, her crumpled body on the other side, I knew something must be really wrong.
She’s one tough bushwalking cookie is our Margot – an experienced, fit and no nonsense kinda gal. So for her to remain on the ground and not even utter a sound, or even cry out, wasn’t a good sign. Her level of toughness, and our utter respect for her, would shine through over the coming hours.
We’d left the MUMC Hut (1600m) (where we’d spent our third and final night for the trip) only 20 minutes earlier and were coming down the North-West Spur of Mt Feathertop. It was early in the day, we were fresh, feeling strong after three days walking and we were carrying much lighter packs, having devoured a mountain of food to equal Feathertop itself.

The track leaves this geodesic dome of wonder and immediately begins a descent of 1140m over 7 kms, to emerge near the Trout Farm in Harrietville. Often overgrown, it hugs the ridge line leading through towering eucalypt forest and regrowth from the 2013 Bushfires. Often steep in parts, it is one of the more difficult and less popular routes to access the popular Mt Feathertop, Razorback Ridge and Federation Hut areas.
We had just breached the tree line and were entering a magnificent Alpine Ash (Eucalyptus delegatensis) forest, in a flat area of respite from the constant slope. After light rain the night before, the ground was covered in damp bark, shed in a continuous lifecycle from the giants that towered above us.
This slippery bark, would be Margot’s un-doing.
So simple. So quick. So unexpected.
So much a reminder of how important appropriate first aid training is for bushwalkers and hikers like us.

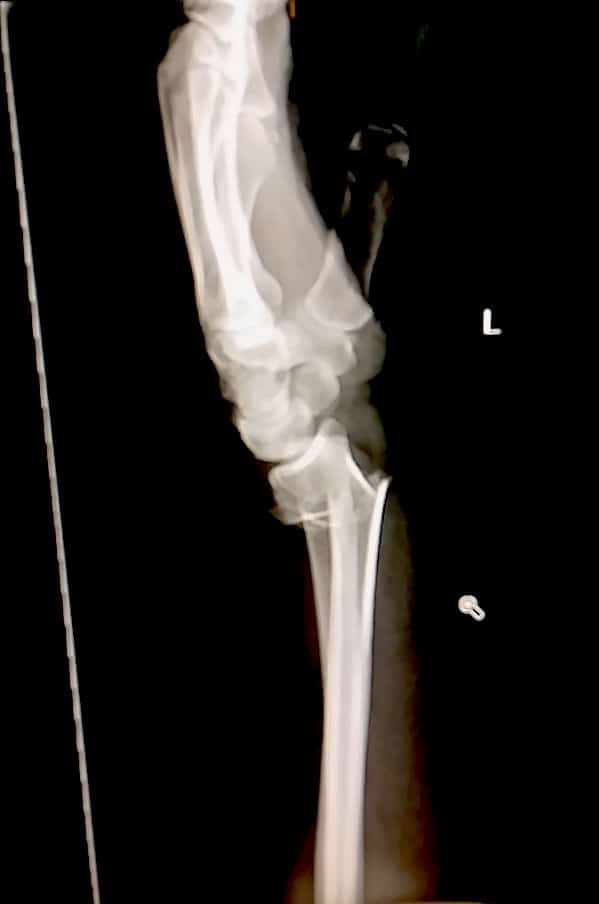
I’ve been doing remote first aid courses for years, always in the hope that I never have to use any of it. But when one of our own goes down, landing awkwardly and snaps their wrist (radius), pushing the broken pieces up into the smaller carpal bones of the hand, I’m so thankful for those endless recertification sessions, every 3 years (12 months for CPR). Practice, practice, practice.
Doing a good quality remote area (or Wilderness) first aid course is ensuring that you pack one of the most essential things into your backpack. It’s packing the knowledge of what to do in a first aid emergency.
And although I’ve whinged in the past, whenever my recertification (recert) comes up, going through the motions of practicing different scenarios, out in the bush, is the only thing that makes the process smoother, easier and automatic.
Doing (and re-doing) remote area first aid courses helps you:
- Stay calm, take control and have well ordered, wise and automatic responses.
- Support the victim, keeping them calm, reduce stress, help them feel taken care of.
- Reduce further injury, setup an injury experience with the best chance of fast recovery.
- Ability to see the bigger picture and delegate roles to other members of the party.
- Share the calm with the rest of the group.
- Create a clear plan and execute it.
- Don’t operate above your pay grade
Here’s the process that we went through to get her to medical help.
In our group of 4, the others knew that I was the most experienced first aider, which made delegation and roles after an emergency happened common knowledge. There’s no question or time wasted with, ‘Who knows first aid? What do we do?
When they called me over and I saw Margot on the ground, I walked calmly and slowly over to her. (Have you ever seen an ambo/paramedic run?). These few seconds gave me the chance to take control of my own reactions to a potentially stressful situation, think clearly and remind myself of my training and slowly unbuckle my own pack to put down.
As Frances told me that it was her wrist, I was slowly lowering my pack and talking to Margot, reassuring her and supporting her wrist as the others helped to remove her waist strap and backpack.
Putting the backpack on it’s side behind her gave her support to sit up and lean back on something, the whole time giving what one of my first aid instructors called, ‘bucket loads of reassurance.’ Speaking calmly with a patient and not ‘over them’ to the people around them is important. They are at the centre of the situation, so include them in discussions and decision making where possible.
Ask questions, how did you do this, what did you land on and checking for other injuries, ie. had she hit her head? Impaled herself on a stick going down? Been bitten by an unseen snake earlier that caused her to become unstable and fall? Try to gauge the level of pain they’re in by using a 1-10 scale, this will help in formulating evacuation plans.
Supporting the injury (and patient) and not causing any further damage meant moving into execution of treatment.
With two other people in the party, Fabulous Frances (FF) and Marvelous Murray (MM), I was able to delegate roles. Making a cup of tea is not only giving sympathy, but helps the patient rehydrate and is a point of comfort in our culture. It also helps people contribute to tasks and not have lots of people hovering around the patient. So whilst FF boiled the billy, I asked MM to find a suitable piece of solid bark to use as a splint. He found an excellent 1cm thick, u-shaped piece, slightly longer than her forearm, that acted as a solid cradle for her arm to sit in. Nice work team. All the while, I was talking with Margot and getting her to support her arm in the place of most comfort (or was that least pain?).
With the splint located, I then used my own piece of foamie mat to pad the bark and Margot’s own piece to protect the sharp end near her elbow. One of Margot’s rolled up triangular bandages provided support under her hand, whilst securing all in place with one of her compression bandages.
Meanwhile, the team were busy with reallocating the items from Margot’s pack into our 3 backpacks, whilst I helped her with taking some Panadol (and an hour later) Ibuprofen.
I felt calm throughout. The only time I felt uneasy was when Margot thought that due to the obvious deformity in her hand, she had dislocated it and asked me to relocate it. Although I’ve received training in relocating a dislocated shoulder in a wilderness environment, I knew nothing about wrists, other than there’s a LOT of bones and things that can go wrong in there. The fact is I’m not a medical professional, I don’t have training in that type of thing, so for me to operate outside of what I’ve been taught would have been ‘above my paygrade’. When it comes to issues of ‘Good Samaritan laws’, it’s generally accepted that if you act within the training that you have received, you minimise your exposure to issues of liability.
When it came to working out an evacuation plan for Margot, ie. trying to work out if we needed to call for backup either medically or for transport (helicopter) it came down to weighing up a few factors.
What did we consider in making a plan?
- Nature of the injury
- Level of pain
- Current weather conditions
- Distance and difficulty to the track head and our car
- Margot’s overall fitness, ability and general state
- Communication options
It can be a tricky balance, working out if a patient is ambulatory or not. Whether to push the button of the PLB or not.
In Margot’s case, where her pain levels were 7-8 yet in good spirits and physically capable otherwise, where the ridge line and mountain above us were covered in low cloud and we were in a densely forested area with multiple canopies, I felt that the best option would be to try to walk her out slowly, re-evaluating if any of these points changed.
And so she did. With a walking pole in her able hand and the rest of us taking her pack and sharing the contents, she headed down 6kms and 900 vertical metres of overgrown, damp track.
With MM up the front, clearing the path as best he could and helping her over fallen trees, whilst FF and I brought up the rear, she wowed us with her tenacity.
She favoured a ‘just keep going’ approach over too many rest stops – she had set her mind to get to the car.
We kept up the constant check-ins with her regarding pain levels and when 4 hrs had passed, offered more Paracetamol and Ibuprofen, along with that priceless prescription of ‘bucketloads of reassurance.’
The ability of humans to ‘hold it together’, when faced with trauma or stressful situations, especially when you can see a definitive light at the end of the tunnel, is remarkable.
Margot was a trooper and did more than hold it together over what must have been a very painful and difficult descent. She continued to hold it together at the Bright Medical Centre, where the Duty Nurse took one look at the photos I’d taken before applying the splint and sling and told her she wasn’t going to touch it, sending her directly to Wangaratta Hospital as it was obviously broken.
And again, at Wangaratta Hospital, where the medical staff praised the splint and sling and finally removed it to X-ray and confirm what we’d suspected. And again, where she went through two reset attempts (only one with local anaesthetic), before being plastered (the drugs were good) and FF drove her to Sydney.
Now, eight weeks later, post surgery with metal plates and screws, she is deep in physiotherapy and reports that her penmanship with her right hand is improving.
In Margot’s own words…
What were your first thoughts after realising that you’d hurt yourself?
It was so quick I don’t remember my left arm hitting the ground at all. But it hurt and when I looked over to it I thought, “Oh no, that is going to need medical attention.” I was lucky to be walking with not only good friends, but people who cope camly and practically in any situation. Everyone was wonderful in helping me down the rest of the spur. I felt bad they had to carry my stuff as I am not good at packing light.
Has the experience made you want to practice your own first aid more? Do another course?
I will definitely be doing another course when I have recovered. It made such a difference having people calmly knowing what to do. I want to be one of those people.
The doctors and nurses at the hospital were very impressed with my improvised splint and remote first aid care. The nurse at the first hospital didn’t even want to unwrap my arm as she thought we had done a better job.
What’s your advice to bushwalkers around first aid?
I think first aid is an important skill to have. When things go wrong we are often in the middle of nowhere with no phone reception and in my case many hours from professional medical help. Even setting off a PLB there could be an hour or 3 before help arrives. In a life threatening situation having some, or all, of your fellow walkers with up to date training could be your only chance of surviving.
What’s your advice to someone giving first aid to an injured person?
Keep calm. Even if you are freaking out on the inside, it makes such a difference if the person giving aid is calm.
What’s the difference between a standard Senior First Aid course and one that is specific for Wilderness or Remote Area First Aid?
It can get pretty confusing with all the different types of courses available and different training companies using words to describe the types of training they offer. Generally speaking, the progression of skills and expertise can be categorised by:
- Senior First Aid (ie. Call 000 and the experts can be here soon to take over)
- Remote Area First Aid (ie. You may not have phone coverage and the experts can’t get there for 30 mins or more)
- Wilderness First Aid (ie. You probably won’t have phone coverage and the experts can’t get there for several hours or more)
- Expedition / First Responder (ie. You’re in a leadership position in charge of other people, for multiple days, in remote/wilderness or expedition conditions, where the experts may be several hours to several days help away).
What’s in my first aid kit?
Check out my article which details everything that’s inside my first aid kit and a few thoughts on why.
Buy an emergency communications device
- BUY a PLB (Personal Locator Beacon) now
- BUY a SPOT Tracker now
- BUY a Garmin InReach Explorer+
- BUY a Garmin InReach Mini